From Surf Wiki (app.surf) — the open knowledge base
Wernicke encephalopathy
Medical condition
Medical condition
| Field | Value |
|---|---|
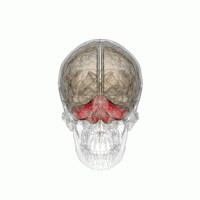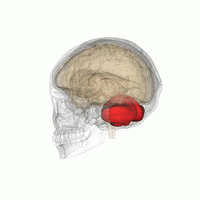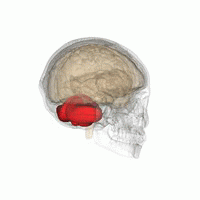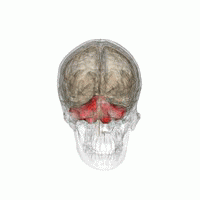
| image | Hypothalamus image.png |
| caption | Hypothalamus |
| synonyms | Wernicke's disease |
| symptoms | Ataxia, ophthalmoplegia, confusion |
| causes | Thiamine deficiency |
| risks | Alcohol use disorder, malnutrition |
Wernicke encephalopathy (WE), also Wernicke's encephalopathy, or wet brain is the presence of neurological symptoms caused by biochemical lesions of the central nervous system after exhaustion of B-vitamin reserves, in particular thiamine (vitamin B1). The condition is part of a larger group of thiamine deficiency disorders that includes beriberi, in all its forms, and alcoholic Korsakoff syndrome. When it occurs simultaneously with alcoholic Korsakoff syndrome it is known as Wernicke–Korsakoff syndrome.
Classically, Wernicke encephalopathy is characterised by a triad of symptoms: ophthalmoplegia, ataxia, and confusion. Around 10% of patients exhibit all three features, and other symptoms may also be present. While it is commonly regarded as a condition particular to malnourished people with alcohol misuse, it can be caused by a variety of diseases. It is treated with thiamine supplementation, which can lead to improvement of the symptoms and often complete resolution, particularly in those where alcohol misuse is not the underlying cause. Often other nutrients also need to be replaced, depending on the cause. Medical literature notes how managing the condition in a timely fashion can avoid worsening symptoms.
Wernicke encephalopathy may be present in the general population with a prevalence of around 2%, and is considered underdiagnosed; probably, many cases are in patients who do not have commonly-associated symptoms.
Signs and symptoms
The classic triad of symptoms found in Wernicke encephalopathy is:
- Ophthalmoplegia: later expanded to include other eye movement disorders; typically affecting the lateral rectus muscle. Lateral nystagmus is the most commonly seen disorder, but lateral rectus palsy—usually bilateral—is common, as well.
- Ataxia: later expanded to include imbalance or any cerebellar dysfunction.
- Confusion: later expanded to include any neuropsychological disturbances. Prevalent in roughly eight in 10 diagnosed cases.
Other possible symptoms include:
- Pupillary changes, Retinal haemorrhage, papilledema, and impaired vision and hearing.
- Fatiguability, apathy, irritability, drowsiness, psychological slowing and/or motor slowing.
- Dysphagia, blushing, sleep apnea, epilepsy and stupor.
- Lactic acidosis.
- Memory impairment, amnesia, depression, and psychosis.
- Hypothermia, polyneuropathy, and hyperhidrosis.
Although hypothermia is usually diagnosed with a body temperature of 35 °C (95 °F) or less, incipient cooling caused by deregulation in the central nervous system (CNS) needs to be monitored because it can promote the development of an infection. The patient may report feeling cold, followed by mild chills, cold skin, moderate pallor, tachycardia, hypertension, tremor, or piloerection. External warming techniques are advised to prevent hypothermia.
Among the frequently altered functions is the cardio-circulatory. There may be tachycardia, dyspnea, chest pain, orthostatic hypotension, changes in heart rate and blood pressure. The lack of thiamine sometimes affects other major energy consumers, the myocardium, and also patients may have developed cardiomegaly. Heart failure with lactic acidosis syndrome has been observed. Cardiac abnormalities are an aspect of the WE, which was not included in the traditional approach, and are not classified as a separate disease. Infections have been pointed out as one of the most frequent triggers of death in WE. Furthermore, infections are usually present in pediatric cases.
In the last stage, other symptoms may occur: hyperthermia, increased muscle tone, spastic paralysis, choreic dyskinesias, and coma.
Because of the frequent involvement of the heart, eyes, and peripheral nervous system, several authors prefer to call it Wernicke disease rather than simply encephalopathy.
Early symptoms are nonspecific, and it has been stated that WE may present nonspecific findings. In Wernicke Korsakoff's syndrome some single symptoms are present in about one-third.
Location of the lesion
Depending on the location of the brain lesion, different symptoms are more frequent:
- Brainstem tegmentum. – Ocular: pupillary changes. Extraocular muscle palsy; gaze palsy: nystagmus.
- Hypothalamus. Medulla: dorsal nuc. of vagus. – Autonomic dysfunction: temperature, cardiocirculatory, respiratory.
- Medulla: vestibular region. Cerebellum. – Ataxia.
- Dorsomedial nuc. of the thalamus. Mammillary bodies. – Amnestic syndrome for recent memory. Mamillary lesions are characteristic-small petechial hemorrhages.
- Diffuse cerebral dysfunction.- Altered cognition: global confusional state.
- Brainstem: periaqueductal gray.- Reduction of consciousness
- Hypothalamic lesions may also affect the immune system, which is known in people who consume excessive amounts of alcohol, causing dysplasias and infections.
Korsakoff syndrome
Korsakoff syndrome, characterised by memory impairment, confabulation, confusion, and personality changes, has a strong and recognised link with WE. A very high percentage of patients with Wernicke–Korsakoff syndrome also have peripheral neuropathy, and many people who consume excess alcohol have this neuropathy without other neurologic signs or symptoms. Korsakoff's occurs much more frequently in WE due to chronic alcoholism. It is uncommon among those who do not consume excessive amounts of alcohol. Up to 80% of WE patients who misuse alcohol develop Korsakoff's syndrome. In Korsakoff's, atrophy of the thalamus and the mammillary bodies and frontal lobe involvement is usually observed. In a study, half of Wernicke–Korsakoff cases had good recovery from the amnesic state, which may take from 2 months to 10 years.
Risk factors
Wernicke encephalopathy has classically been thought of as a disease solely of people who drink excessive amounts of alcohol, but it is also found in the chronically undernourished, and in recent years has been discovered post bariatric surgery. Without being exhaustive, the documented causes of Wernicke encephalopathy have included:
- pancreatitis, liver dysfunction, chronic diarrhea, celiac disease, Crohn's disease, uremia,
- vomiting, hyperemesis gravidarum, malabsorption, gastrointestinal surgery or diseases
- incomplete parenteral nutrition, starvation/fasting
- chemotherapy, renal dialysis, diuretic therapy, stem cell/marrow transplantation
- cancer, AIDS, Creutzfeldt–Jakob disease, febrile infections
- this disease may even occur in some people with normal, or even high blood thiamine levels, or people with deficiencies in intracellular transport of this vitamin. Selected genetic mutations, including presence of the X-linked transketolase-like 1 gene, SLC19A2 thiamine transporter protein mutations, and the aldehyde dehydrogenase-2 gene, which may predispose to alcohol use disorder. The APOE epsilon-4 allele, involved in Alzheimer's disease, may increase the chance of developing neurological symptoms.
Pathophysiology
Thiamine deficiency and errors of thiamine metabolism are believed to be the primary cause of Wernicke encephalopathy. Thiamine, also called B1, helps to break down glucose. Specifically, it acts as an essential coenzyme to the TCA cycle and the pentose phosphate shunt. Thiamine is first metabolised to its more active form, thiamine diphosphate (TDP), before it is used. The body only has 2–3 weeks of thiamine reserves, which are readily exhausted without intake, or if depletion occurs rapidly, such as in chronic inflammatory states or in diabetes.
- Metabolism of carbohydrates, releasing energy.
- Production of neurotransmitters including glutamic acid and GABA.
- Lipid metabolism, necessary for myelin production.
- Amino acid modification. Probably linked to the production of taurine, of great cardiac importance.
Neuropathology
The primary neurological-related injury caused by thiamine deficiency in WE is three-fold: oxidative damage, mitochondrial injury leading to apoptosis, and directly stimulating a pro-apoptotic pathway. Thiamine deficiency affects both neurons and astrocytes, glial cells of the brain. Thiamine deficiency alters the glutamate uptake of astrocytes, through changes in the expression of astrocytic glutamate transporters EAAT1 and EAAT2, leading to excitotoxicity. Other changes include those to the GABA transporter subtype GAT-3, GFAP, glutamine synthetase, and the Aquaporin 4 channel. Focal lactic acidosis also causes secondary oedema, oxidative stress, inflammation and white matter damage.
Pathological anatomy

Despite its name, WE is not related to Wernicke's area, a region of the brain associated with speech and language interpretation.
Brain lesions in WE are usually credited to focal lactic acidosis. An absence of thiamine can lead to too much pyruvate within the cells since it is not available to help convert pyruvate through the TCA cycle. An increase in pyruvate causes an increase in lactate concentration leading to focal lactic acidosis.
Lesions can be reversed in most cases with immediate supplementation of thiamine.
Lesions are usually symmetrical in the periventricular region, diencephalon, the midbrain, hypothalamus, and cerebellar vermis. Brainstem lesions may include cranial nerve III, IV, VI and VIII nuclei, the medial thalamic nuclei, and the dorsal nucleus of the vagus nerve. Oedema may be found in the regions surrounding the third ventricle, and fourth ventricle, also appearing petechiae and small hemorrhages. Chronic cases can present the atrophy of the mammillary bodies.
In 1949, the idea that WE lesions are a result of a disruption to the blood-brain barrier was introduced. Large proteins passing into the brain can put neurological tissue at risk of toxic effects. The blood-brain barrier junctions are typically found to have WE lesions located at that region of the brain.
An altered blood–brain barrier may cause a perturbed response to certain drugs and foods.
Diagnosis
Diagnosis of Wernicke encephalopathy or disease is made clinically. Caine et al. in 1997 established criteria that Wernicke encephalopathy can be diagnosed in any patient with just two or more of the main symptoms noted above. The sensitivity of the diagnosis by the classic triad was 23% but increased to 85% taking two or more of the four classic features. These criteria are challenged because all the cases he studied were people who drank excessive amounts of alcohol. Some consider it sufficient to suspect the presence of the disease with only one of the principal symptoms.
The sensitivity of magnetic resonance imaging (MR) was 53% and the specificity was 93%. The reversible cytotoxic edema was considered the most characteristic lesion of WE. The location of the lesions were more frequently atypical among people who drank appropriate amounts of alcohol, while typical contrast enhancement in the thalamus and the mammillary bodies was observed frequently associated with alcohol misuse. These abnormalities may include:
- Dorsomedial thalami, periaqueductal gray matter, mamillary bodies, tectal plate and brainstem nuclei are commonly affected. Involvement is always bilateral and symmetric. Value of DWI in the diagnosis of WE is minimal. Axial FLAIR MRI images represent the best diagnostic MRI sequence. Contrast material may highlight involvement of the mamillary bodies. There appears to be very little value for CT scans.
Thiamine can be measured using an erythrocyte transketolase activity assay, or by activation by measurement of in vitro thiamine diphosphate levels. Normal thiamine levels do not necessarily rule out the presence of WE, as this may be a patient with difficulties in intracellular transport.
Prevention
There are hospital protocols for prevention, supplementing with thiamine in the presence of: history of alcohol misuse or related seizures, requirement for IV glucose, signs of malnutrition, poor diet, recent diarrhea or vomiting, peripheral neuropathy, intercurrent illness, delirium tremens or treatment for DTs, and others.
Some experts advise parenteral thiamine should be given to all at-risk patients in the emergency department.
In the clinical diagnosis should be remembered that early symptoms are nonspecific, and it has been stated that WE may present nonspecific findings.
In some countries certain foods have been supplemented with thiamine, and have reduced WE cases. Improvement is difficult to quantify because they applied several different actions. Avoiding or moderating alcohol consumption and having adequate nutrition reduces one of the main risk factors in developing Wernicke–Korsakoff syndrome..
Treatment
Most symptoms will improve quickly if deficiencies are treated early. Memory disorder may be permanent.
In patients suspected of WE, thiamine treatment should be started immediately. two or three times daily. Thiamine administration is usually continued until clinical improvement ceases.
Considering the diversity of possible causes and several surprising symptomatologic presentations, and because there is low assumed risk of toxicity of thiamine, because the therapeutic response is often dramatic from the first day, some qualified authors indicate parenteral thiamine if WE is suspected, both as a resource for diagnosis and treatment. Parenteral thiamine administration is associated with a very small risk of anaphylaxis.
People who consume excessive amounts of alcohol may have poor dietary intakes of several vitamins, and impaired thiamine absorption, metabolism, and storage; they may thus require higher doses.
If glucose is given, such as in people with an alcohol use disorder who are also hypoglycaemic, thiamine must be given concurrently. If this is not done, the glucose will rapidly consume the remaining thiamine reserves, exacerbating this condition.
The observation of edema in MR, and also the finding of inflation and macrophages in necropsied tissues, has led to successful administration of antiinflammatories.
Other nutritional abnormalities should also be looked for, as they may be exacerbating the disease. In particular, magnesium, a cofactor of transketolase which may induce or aggravate the disease.
Other supplements may also be needed, including: cobalamin, ascorbic acid, folic acid, nicotinamide, zinc, phosphorus (dicalcium phosphate) and in some cases taurine, especially suitable when there cardiocirculatory impairment. Patient-guided nutrition is suggested. In patients with Wernicke–Korsakoff syndrome, even higher doses of parenteral thiamine are recommended. Concurrent toxic effects of alcohol should also be considered.
Epidemiology
There are no conclusive statistical studies, all figures are based on partial studies.
Wernicke's lesions were observed in 0.8 to 2.8% of the general population autopsies, and 12.5% of people with an alcohol use disorder. This figure increases to 35% of such individuals if including cerebellar damage due to lack of thiamine.
Most autopsy cases were from people with an alcohol use disorder. Autopsy series were performed in hospitals on the material available which is unlikely to be representative of the entire population. Considering the slight affectations, previous to the generation of observable lesions at necropsy, the percentage should be higher. There is evidence to indicate that Wernicke encephalopathy is underdiagnosed. For example, in one 1986 study, 80% of cases were diagnosed postmortem. Is estimated that only 5–14% of patients with WE are diagnosed in life.
In a series of autopsy studies held in Recife, Brazil, it was found that only 7 out of 36 had consumed excessive amounts of alcohol, and only a small minority had malnutrition. In a reviewed of 53 published case reports from 2001 to 2011, the relationship with alcohol was also about 20% (10 out of 53 cases).
WE related to alcohol misuse is more common in males and is more common in females when not related to alcohol misuse. In alcohol-related cases, WE patients average the age of 40, and non-alcohol-related cases typically occur in younger people.
History
WE was first identified in 1881 by the German neurologist Carl Wernicke, although the link with thiamine was not identified until the 1930s.
Carl Wernicke discovered the sensory center of speech. Wernicke figured out that Broca's area was not the only center of speech, it was also able to distinguish motor aphasia from sensory aphasia. He also pointed to the possibility of conduction aphasia since he came to understand the arrangement of the brain's extrinsic and intrinsic connections. He demonstrated that the sensory information reached its corresponding area in the cerebral cortex through projection fibers. From there, this information, following the association system, would be distributed to different regions of the cortex, integrating sensory processing.
He reported three patients with WE, including two men (aged 33 and 36) who were alcoholics and one woman (aged 20) who ingested sulfuric acid, leading to pyloric stenosis. All three had ocular motor abnormalities and he performed an autopsy on each, providing a clinical-pathological correlation.
A similar presentation of this disease was described by the Russian psychiatrist Sergei Korsakoff in a series of articles published 1887–1891; where the chronic version of WE was described as Korsakoff's Syndrome, involving symptoms of amnesia.
References
References
- "Wernicke Encephalopathy". U.S. National Library of Medicine.
- (December 2022). "Wernicke-Korsakoff syndrome diagnostics and rehabilitation in the post-acute phase". Addiction Neuroscience.
- (July 2013}}{{cite journal). "Wernicke's encephalopathy and Korsakoff's syndrome revisited". Neuropsychology Review.
- Ropper A, Brown R. Princ. of Neurology, Adams & Victor. 8º ed. McGraw Hill 2007.
- (2000). "Prevention and treatment of Wernicke-Korsakoff syndrome". Alcohol and Alcoholism.
- (May 2007). "Wernicke's encephalopathy: new clinical settings and recent advances in diagnosis and management". The Lancet. Neurology.
- (December 2010). "EFNS guidelines for diagnosis, therapy and prevention of Wernicke encephalopathy". European Journal of Neurology.
- (2021-01-01). "Chapter 29 – The contribution of mamillary body damage to Wernicke's encephalopathy and Korsakoff's syndrome". Elsevier.
- (July 2021). "Wernicke-Korsakoff syndrome despite no alcohol abuse: A summary of systematic reports". Journal of the Neurological Sciences.
- (2012). "Wernicke-Korsakoff-syndrome: under-recognized and under-treated". Psychosomatics.
- (June 2012). "Wernicke's encephalopathy: expanding the diagnostic toolbox". Neuropsychology Review.
- (June 1989). "Papilloedema delaying diagnosis of Wernicke's encephalopathy in a comatose patient". Postgraduate Medical Journal.
- (May 2012). "Wernicke's encephalopathy with visual loss in a patient with hyperemesis gravidarum". The Journal of the Association of Physicians of India.
- (August 2008). "Hearing and seeing: Unusual early signs of Wernicke encephalopathy". Neurology.
- (2012). "Acute Wernicke encephalopathy and sensorineural hearing loss complicating bariatric surgery". Connecticut Medicine.
- (1994). "Tratado de Neurología". Editorial Libro del Año.
- (March 2010). "EFNS guideline on the management of status epilepticus in adults". European Journal of Neurology.
- (August 1996). "Severe acute metabolic acidosis and Wernicke's encephalopathy following chemotherapy with 5-fluorouracil and cisplatin: case report and review of the literature". Japanese Journal of Clinical Oncology.
- (1990). "Characteristics of the memory loss of a patient with Wernicke-Korsakoff's syndrome without alcoholism". Neuropsychologia.
- (January 2013). "Thiamine nutritional status and depressive symptoms are inversely associated among older Chinese adults". The Journal of Nutrition.
- (2006). "Wernicke's encephalopathy after gastric bypass that masqueraded as acute psychosis: a case report". Current Surgery.
- (January 2006). "Acute psychotic disorder after gastric bypass surgery: differential diagnosis and treatment". The American Journal of Psychiatry.
- (June 2000). "Australian experience with the Wernicke-Korsakoff syndrome". Addiction.
- (April 1990). "Wernicke's encephalopathy". American Family Physician.
- (1987). "[Hypothermia in Wernicke's encephalopathy]". Revue Neurologique.
- (June 2014). "Color Atlas of Neurology". Thieme }}{{page needed.
- (2008). "The Interface of Neurology & Internal Medicine". Wolters Kluwer Health/Lippincott Williams & Wilkins.
- (2004). "Color Atlas of Neurology". Thieme.
- (September 2009). "[Case of Wernicke's encephalopathy and subacute combined degeneration of the spinal cord due to vitamin deficiency showing changes in the bilateral corpus striatum and cardiac arrest due to beriberi heart disease]". Brain and Nerve = Shinkei Kenkyu No Shinpo.
- (March 1995). "An international perspective on the prevalence of the Wernicke-Korsakoff syndrome". Metabolic Brain Disease.
- (April 1999). "Early diagnosis of pediatric Wernicke's encephalopathy". Pediatric Neurology.
- (February 2005). "Outbreak of life-threatening thiamine deficiency in infants in Israel caused by a defective soy-based formula". Pediatrics.
- (November 2022). "Thiamin Deficiency". Merk Manuals.
- (May 2007). "Wernicke's encephalopathy: new clinical settings and recent advances in diagnosis and management". The Lancet. Neurology.
- (October 2003). "Guidelines for the Treatment of Alcohol Problems". National Drug and Alcohol Research Centre, Commonwealth of Australia.
- (2007). "Clinical neuropathology: text and color atlas". Demos Medical Publishing.
- (June 2012). "The evolution and treatment of Korsakoff's syndrome: out of sight, out of mind?". Neuropsychology Review.
- (2007). "Cecil Medicine". Saunders, Elsevier.
-
- Wernicke-Korsakoff syndrome
- (April 2013). "The role of thiamine in HIV infection". International Journal of Infectious Diseases.
- (May 2011). "Severe encephalopathy, lactic acidosis, vegetative instability and neuropathy with 5-Fluorouracil treatment – pyrimidine degradation defect or beriberi?". Case Reports in Oncology.
- (October 2009). "Micronutrient deficiencies an unmet need in heart failure". Journal of the American College of Cardiology.
- (2011). "Nutritional assessment in heart failure patients". Congestive Heart Failure.
- (2012). "New considerations on the neuromodulatory role of thiamine". Pharmacology.
- (2009). "Astrocytes are a major target in thiamine deficiency and Wernicke's encephalopathy". Neurochemistry International.
- (June 1998). "Mechanisms of neuronal cell death in Wernicke's encephalopathy". Metabolic Brain Disease.
- (January 2021). "Don't seek, don't find: The diagnostic challenge of Wernicke's encephalopathy". Annals of Clinical Biochemistry: International Journal of Laboratory Medicine.
- (February 2009). "Neuroimaging findings in acute Wernicke's encephalopathy: review of the literature". AJR. American Journal of Roentgenology.
- (August 2015}}{{MEDRS). ["Wernicke's Disease (or Wernicke's Encephalopathy). Symptoms and new treatments. Clinical and practical approach. Daily monitoring for twelve years of a reversed severe case."](http://enfermedad-de-wernicke.weebly.com/}} {{self-published inline).
- (2011-09-12). "Current medical diagnosis & treatment 2012". McGraw-Hill Medical.
- (January 1997). "Operational criteria for the classification of chronic alcoholics: identification of Wernicke's encephalopathy". Journal of Neurology, Neurosurgery, and Psychiatry.
- "Protocol for: The management of the alcohol withdrawal syndrome and Wernicke encephalopathy". East Kent Hospitals NHS Trust.
- (2011). "Differential diagnosis for bilateral abnormalities of the basal ganglia and thalamus". Radiographics.
- (June 2012). "Clinical Guideline: The Management of Wernicke's Encephalopathy (WE)". Guy's and St. Thomas Hospitals.
- (June 2006). "Guidelines for the Management of Alcohol Issues in the Acute Hospital Setting". Doncaster and Bassetlaw Hospitals.
- Thomson A, Guerrini I, Marshall EJ. "Incidence of Adverse Reactions to Parenteral Thiamine in the Treatment of Wernicke's Encephalopathy, and Recommendations." ''Alcohol and Alcoholism.'' 2019 Nov;54(6):609-614. doi:https://doi.org/10.1093/alcalc/agy091
- (2009). "Current Medical Diagnosis & Treatment 2012". McGraw-Hill Medical.
- (March 2003). "Principles and Practice of Neuropathology". Oxford University Press.
- (June 1994). "[Beneficial effect of steroid pulse therapy on Wernicke-Korsakoff syndrome due to hyperemesis gravidarum]". Rinsho Shinkeigaku = Clinical Neurology.
- (February 1962). "[Corticotherapy of the severe forms of the Gayet-Wernicke encephalopathy]". Lille Medical.
- (2007). "Principios de neurología de Adams y Victor". McGraw-Hill.
- (2007). "Neurologia.". Harcourt Brace De Espana SA.
- (2002). "Medicina Interna".
- (1990). "Medicina Interna". Médica Panamericana.
- (2002). "The Royal College of Physicians report on alcohol: guidelines for managing Wernicke's encephalopathy in the accident and Emergency Department". Alcohol and Alcoholism.
- (2002). "Taurine: a conditionally essential amino acid in humans? An overview in health and disease". Nutricion Hospitalaria.
- (June 1994). "[Beneficial effect of steroid pulse therapy on Wernicke-Korsakoff syndrome due to hyperemesis gravidarum]". Rinsho Shinkeigaku = Clinical Neurology.
- (November 1982). "Brain lesions in alcoholics. A neuropathological study with clinical correlations". Journal of the Neurological Sciences.
- (April 1986). "Clinical signs in the Wernicke-Korsakoff complex: a retrospective analysis of 131 cases diagnosed at necropsy". Journal of Neurology, Neurosurgery, and Psychiatry.
- (March 1979). "Wernicke's encephalopathy: a more common disease than realised. A neuropathological study of 51 cases". Journal of Neurology, Neurosurgery, and Psychiatry.
- (July 1992). "Korsakoff minus Wernicke syndrome". Alcohol and Alcoholism (Oxford, Oxfordshire).
- (September 1992). "Coma and death in unrecognized Wernicke's encephalopathy. An autopsy study". Arquivos de Neuro-Psiquiatria.
- (2021-06-28). "The anatomy of the brain – learned over the centuries". Surgical Neurology International.
- (2020-06-30). "Neuro-ophthalmic Manifestations of Wernicke Encephalopathy". Eye and Brain.
- (2012-11-01). "Wernicke-Korsakoff-syndrome: under-recognized and under-treated". Psychosomatics.
- (May 2007). "Wernicke's encephalopathy: new clinical settings and recent advances in diagnosis and management". The Lancet. Neurology.
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Wernicke encephalopathy — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report