From Surf Wiki (app.surf) — the open knowledge base
Pelvic congestion syndrome
| Field | Value |
|---|---|
| name | Pelvic venous disease |
| synonyms | Pelvic congestion syndrome, Pelvic venous insufficiency, Pelvic varicocele syndrome |
| image | 9cmFibroidPelvicCongestionS.png |
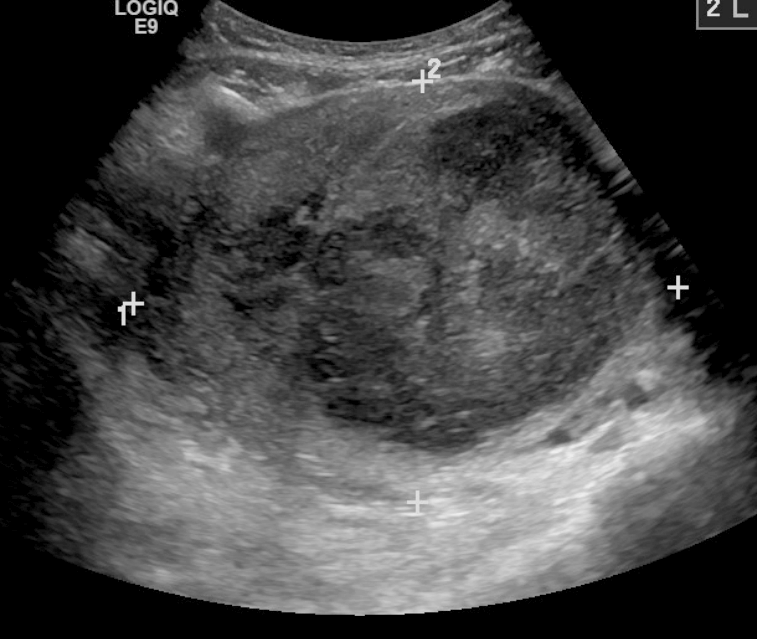
| caption | A very large (9 cm) fibroid of the uterus which is causing pelvic congestion syndrome as seen on X-ray computed tomography |
| field | Interventional Radiology, gynecology |
| symptoms | Chronic pelvic pain, lower back pain, leg pain, dyspareunia, dysmenorrhea |
| complications | Chronic pain, varicose veins in lower extremities, mood disturbances |
| onset | Typically premenopausal women, often after multiple pregnancies |
| duration | Chronic |
| types | Primary (due to vein insufficiency) and Secondary (due to external compression) |
| causes | Hormonal influences, vein valve dysfunction, increased pelvic blood flow from pregnancy |
| risks | Multiple pregnancies, hormonal imbalances, family history, varicose veins |
| diagnosis | Ultrasound, CT scan, MRI, Pelvic venography, Laparoscopy |
| differential | Endometriosis, Irritable Bowel Syndrome, Interstitial Cystitis |
| prevention | None specific, but early diagnosis and management are beneficial |
| treatment | Hormonal therapy, Ovarian vein embolization, Sclerotherapy, pain management, compression garments |
| medication | Medroxyprogesterone, Nonsteroidal anti-inflammatory drugs (NSAIDs), Gonadotropin-releasing hormone agonists |
| prognosis | Often favorable with treatment; ~70-80% symptom relief post-embolization |
| frequency | 30% of women presenting complaints of chronic pelvic pain |
| deaths | Rare |
Pelvic congestion syndrome, also known as pelvic vein incompetence, is a long-term condition believed to be due to enlarged veins in the lower abdomen. The condition may cause chronic pain, such as a constant dull ache, which can be worsened by standing or sex. Pain in the legs or lower back may also occur.
While the condition is believed to be due to blood flowing back into pelvic veins as a result of faulty valves in the veins, this hypothesis is not certain. The condition may occur or worsen during pregnancy. The presence of estrogen is believed to be involved in the mechanism. Diagnosis may be supported by ultrasound, CT scan, MRI, or laparoscopy.
Early treatment options include medroxyprogesterone or nonsteroidal anti-inflammatory drugs (NSAIDs). While pelvic venous insufficiency was identified in the 1850s it was only linked with pelvic pain in the 1940s.
Signs and symptoms
Women with this condition experience a constant pain that may be dull and aching, but is occasionally more acute. The pain is worse at the end of the day and after long periods of standing, and those affected get relief when they lie down. The pain is worse during or after sexual intercourse, and can be worse just before the onset of the menstrual period.
Women with pelvic congestion syndrome have a larger uterus and a thicker endometrium. 56% of women manifest cystic changes to the ovaries, and many report other symptoms, such as dysmenorrhea, back pain, vaginal discharge, abdominal bloating, mood swings or depression, and fatigue.
Causes
- Local pelvic hormonal milieu
- Venous outflow obstruction, such as May-Thurner syndrome, Nutcracker syndrome, Budd-Chiari syndrome, or left renal vein thrombosis
- External compression due to tumor (including fibroids, endometriosis), or scarring
Diagnosis

Diagnosis can be made using ultrasound or laparoscopy testing. The condition can also be diagnosed with a venogram, CT scan, or an MRI. Ultrasound is the diagnostic tool most commonly used.
Treatment
Early treatment options include pain medication using nonsteroidal anti-inflammatory drugs, and suppression of ovarian function.
More advanced treatment includes a minimally invasive procedure performed by an Interventional Radiologist. This minimally invasive procedure involves stopping blood within the pelvic varicose veins using a minimally invasive procedure called a catheter directed embolization. The procedure rarely requires an overnight stay in hospital and is usually performed as an outpatient procedure, and is done using local anesthetic and moderate sedation.
References
References
- (2023). "Pelvic Congestion Syndrome: Causes, Symptoms & Treatment".
- "Pelvic Congestion Syndrome".
- (March 2018). "Pelvic Congestion Syndrome: Systematic Review of Treatment Success.". Seminars in Interventional Radiology.
- (2020). "Pelvic Congestion Syndrome". Statpearls.
- "Pelvic Congestion Syndrome - Women's Health Issues".
- (January 2016). "The relationship between pelvic vein incompetence and chronic pelvic pain in women: systematic reviews of diagnosis and treatment effectiveness.". [[Health Technology Assessment (journal).
- (March 2018). "Pelvic Congestion Syndrome: Systematic Review of Treatment Success.". Seminars in Interventional Radiology.
- (December 2008). "Dysmenorrhea". Merck Online Medical Manual.
- Phillip Reginald, MD. "Pelvic Congestion". The International Pelvic Pain Society.
- (2014). "Rutherford's vascular surgery references.". Elsevier Saunders.
- (Oct 2014). "Transvaginal duplex ultrasonography appears to be the gold standard investigation for the haemodynamic evaluation of pelvic venous reflux in the ovarian and internal iliac veins in women.". Phlebology.
- "Pelvic Pain (Pelvic Congestion Syndrome)". Johns Hopkins Medicine.
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Pelvic congestion syndrome — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report