From Surf Wiki (app.surf) — the open knowledge base
Cervix
Lower part of the uterus in the female reproductive system
Lower part of the uterus in the female reproductive system
| Field | Value |
|---|---|
| Name | Uterine cervix |
| Latin | cervix uteri |
| Image | Cervix_svg_hariadhi.svg |
| Caption | Human cervix |
| Image2 | Scheme_female_reproductive_system-en.svg |
| Caption2 | Diagram of the female human reproductive tract |
| Precursor | Paramesonephric ducts |
| Artery | Vaginal artery and uterine artery |
The cervix (: cervices) or uterine cervix () is a dynamic fibromuscular sexual organ of the female reproductive system that connects the vagina with the uterine cavity. The human female cervix has been documented anatomically since at least the time of Hippocrates, over 2,000 years ago. The cervix is approximately 4 cm long with a diameter of approximately 3 cm and tends to be described as a cylindrical shape, although the front and back walls of the cervix are contiguous. The size of the cervix changes throughout a female's life cycle. For example, females in the fertile years of their reproductive cycle tend to have larger cervixes than postmenopausal females; likewise, females who have produced offspring have a larger cervix than those who have not.
In relation to the vagina, the part of the cervix that opens into the uterus is called the internal os while the opening of the cervix into the vagina is called the external os. Between those extremes is the conduit commonly called the cervical canal. The lower part of the cervix, known as the vaginal portion of the cervix (or ectocervix), bulges into the top of the vagina. The endocervix borders the uterus. The cervical conduit has at least two types of epithelium (lining): the endocervical lining is glandular epithelia that lines the endocervix with a single layer of column-shaped cells; while the ectocervical part of the conduit contains squamous epithelium. Squamous epithelia line the conduit with multiple layers of cells topped with flat cells. These two linings converge at the squamocolumnar junction (SCJ). This junction changes location dynamically throughout a female's life. The cervix is the organ that allows epithelia to flow from a female's uterus and out through their vagina at menstruation. Menstruation releases epithelia from a female’s uterus with every period of their fertile years, unless pregnancy occurs.
Several methods of contraception aim to prevent fertilization by blocking the conduit, including cervical caps and cervical diaphragms, preventing the passage of sperm through the cervix. Other approaches include methods that observe cervical mucus, such as the Creighton Model and Billings method. Cervical mucus's consistency changes during menstrual periods, which may signal ovulation.
During vaginal childbirth, the cervix must flatten and dilate to allow the foetus to progress along the birth canal. Midwives and doctors use the extent of cervical dilation to assist decision-making during childbirth.
Cervical infections with the human papillomavirus (HPV) can cause changes in the epithelium, which can lead to cancer of the cervix. Cervical cytology tests can detect cervical cancer and its precursors to enable early, successful treatment. Ways to avoid HPV include avoiding heterosexual sex, using penile condoms, and receiving the HPV vaccination.
Structure
The cervix is part of the female reproductive system. Around 2–3 cm in length, and the mucosa covering the ectocervix is known as the exocervix. The cervix has an inner mucosal layer, a thick layer of smooth muscle, and posteriorly the supravaginal portion has a serosal covering consisting of connective tissue and overlying peritoneum.


In front of the upper part of the cervix lies the bladder, separated from it by cellular connective tissue known as parametrium, which also extends over the sides of the cervix. To the rear, the supravaginal cervix is covered by peritoneum, which runs onto the back of the vaginal wall and then turns upwards and onto the rectum, forming the recto-uterine pouch.
The cervical canal varies greatly in length and width between women or throughout a woman's life, and it can measure 8 mm (0.3 inch) at its widest diameter in premenopausal adults. It is wider in the middle and narrower at each end. The anterior and posterior walls of the canal each have a vertical fold, from which ridges run diagonally upwards and laterally. These are known as palmate folds, due to their resemblance to a palm leaf. The anterior and posterior ridges are arranged so that they interlock with each other and close the canal. They are often effaced after pregnancy.
The ectocervix (also known as the vaginal portion of the cervix) has a convex, elliptical shape and projects into the cervix between the anterior and posterior vaginal fornices. On the rounded part of the ectocervix is a small, depressed external opening, connecting the cervix with the vagina. The size and shape of the ectocervix and the external opening (external os) can vary according to age, hormonal state, and whether childbirth has taken place. In women who have not had a vaginal delivery, the external opening is small and circular, and in women who have had a vaginal delivery, it is slit-like. On average, the ectocervix is 3 cm long and 2.5 cm wide.
Blood is supplied to the cervix by the descending branch of the uterine artery and drains into the uterine vein. The pelvic splanchnic nerves, emerging as S2–S3, transmit the sensation of pain from the cervix to the brain. These nerves travel along the uterosacral ligaments, which pass from the uterus to the anterior sacrum.
Three channels facilitate lymphatic drainage from the cervix. The anterior and lateral cervix drains to nodes along the uterine arteries, travelling along the cardinal ligaments at the base of the broad ligament to the external iliac lymph nodes and ultimately the paraaortic lymph nodes. The posterior and lateral cervix drains along the uterine arteries to the internal iliac lymph nodes and ultimately the paraaortic lymph nodes, and the posterior section of the cervix drains to the obturator and presacral lymph nodes. However, there are variations as lymphatic drainage from the cervix travels to different sets of pelvic nodes in some people. This has implications in scanning nodes for involvement in cervical cancer.
After menstruation and directly under the influence of estrogen, the cervix undergoes a series of changes in position and texture. During most of the menstrual cycle, the cervix remains firm and is positioned low and closed. However, as ovulation approaches, the cervix becomes softer and rises to open in response to the higher levels of estrogen present. These changes are also accompanied by changes in cervical mucus, described below.
Development
As a component of the female reproductive system, the cervix is derived from the two paramesonephric ducts (also called Müllerian ducts), which develop around the sixth week of embryogenesis. During development, the outer parts of the two ducts fuse, forming a single urogenital canal that will become the vagina, cervix and uterus. The cervix grows in size at a smaller rate than the body of the uterus, so the relative size of the cervix over time decreases, decreasing from being much larger than the body of the uterus in fetal life, twice as large during childhood, and decreasing to its adult size, smaller than the uterus, after puberty. New studies show, however, that all the cervical as well as large part of the vaginal epithelium are derived from Müllerian duct tissue and that phenotypic differences might be due to other causes.
Histology
Transformation zone
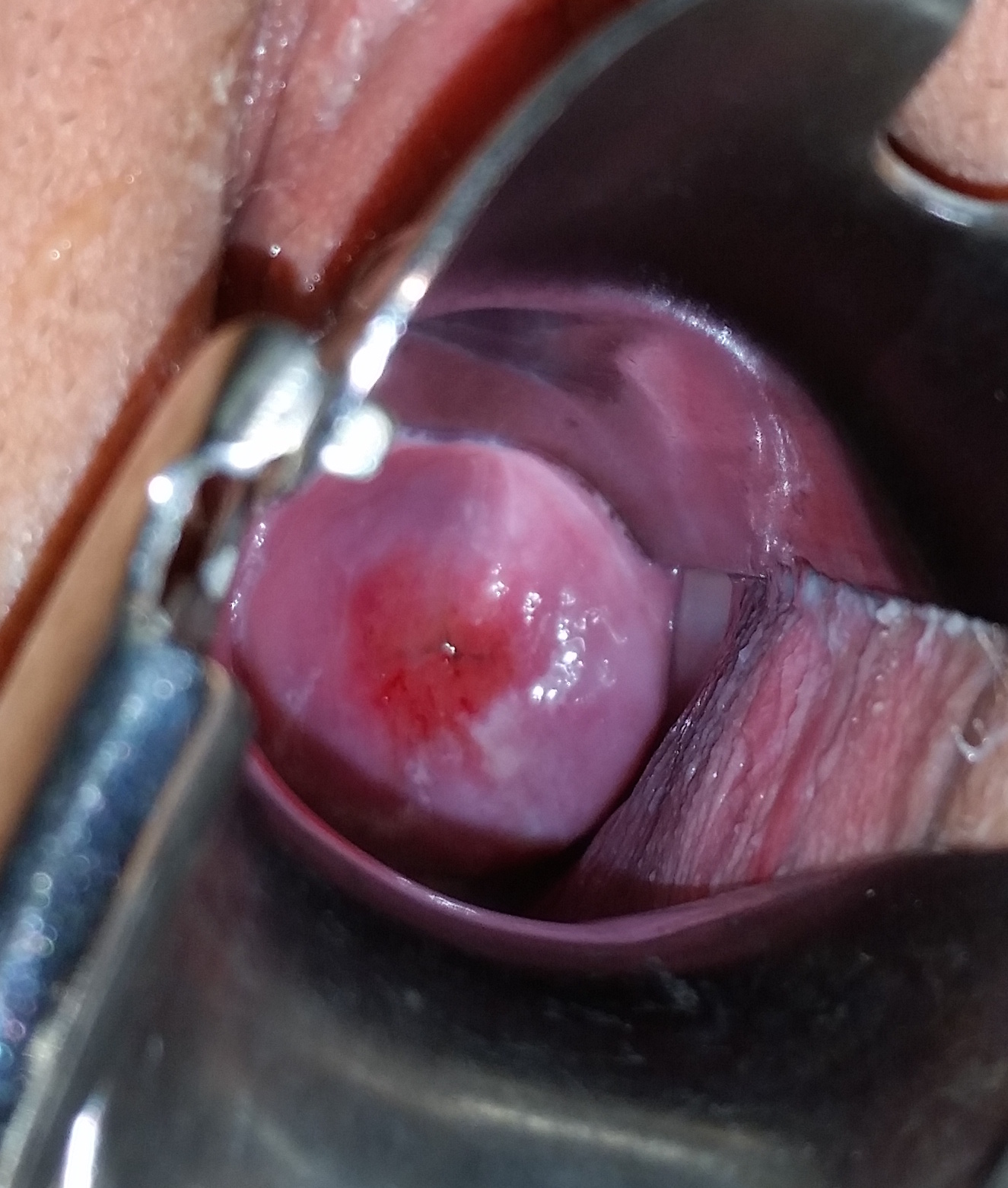
The endocervical mucosa is about 3 mm thick and lined with a single layer of columnar mucous cells. It contains numerous tubular mucous glands, which empty viscous alkaline mucus into the lumen. Underlying both types of epithelium is a tough layer of collagen. The mucosa of the endocervix is not shed during menstruation. The cervix has more fibrous tissue, including collagen and elastin, than the rest of the uterus. File:Cervix Normal Squamocolumnar Junction (565238127).jpg|The squamocolumnar junction of the cervix, with abrupt transition: The ectocervix, with its stratified squamous epithelium, is visible on the left. Simple columnar epithelium, typical of the endocervix, is visible on the right. A layer of connective tissue is visible under both types of epithelium. File:Transformation zone types.png|Transformation zone types: Type 1: Completely ectocervical (common under hormonal influence). Type 2: Endocervical component but fully visible (common before puberty). Type 3: Endocervical component, not fully visible (common after menopause). In prepubertal girls, the functional squamocolumnar junction is just within the cervical canal.
After menopause, the uterine structures involute, and the functional squamocolumnar junction moves into the cervical canal.
Nabothian cysts (or Nabothian follicles) form in the transformation zone where the lining of metaplastic epithelium has replaced mucous epithelium and caused a strangulation of the outlet of some of the mucous glands. A buildup of mucus in the glands forms Nabothian cysts, usually less than about 5 in diameter, which are considered physiological rather than pathological. Both gland openings and Nabothian cysts are helpful to identify the transformation zone.
Function
Fertility
The cervical canal is a pathway through which sperm enter the uterus after being induced by estradiol after penile-vaginal intercourse, and some forms of artificial insemination. Some sperm remains in cervical crypts, infoldings of the endocervix, which act as a reservoir, releasing sperm over several hours and maximising the chances of fertilisation. A theory states the cervical and uterine contractions during orgasm draw semen into the uterus.
Some methods of fertility awareness, such as the Creighton model and the Billings method involve estimating a woman's periods of fertility and infertility by observing physiological changes in her body. Among these changes are several involving the quality of her cervical mucus: the sensation it causes at the vulva, its elasticity (Spinnbarkeit), its transparency, and the presence of ferning.
Cervical mucus
Several hundred mucus-secreting crypts in the endocervix produce 20–60 mg of cervical mucus a day, increasing to 600 mg around the time of ovulation. The viscosity and water content vary during the menstrual cycle; cervical mucus is composed of around 93% water, reaching 98% at midcycle. It contains electrolytes such as calcium, sodium, and potassium; organic components such as glucose, amino acids, and soluble proteins; trace elements including zinc, copper, iron, manganese, and selenium; free fatty acids; enzymes such as amylase; and prostaglandins. Its consistency is determined by the influence of the hormones estrogen and progesterone. In the follicular phase of the menstrual cycle, estrogen dominates and cervical mucus gradually becomes thinner, hitting its lowest viscosity at ovulation. At midcycle, around the time of ovulation—a period of high estrogen levels— the mucus is thin and serous to allow sperm to enter the uterus and is more alkaline and, hence, more hospitable to sperm.
At other times in the cycle, the mucus is thick and more acidic due to the effects of progesterone. Women taking an oral contraceptive pill also have thick mucus from the effects of progesterone.
A cervical mucus plug, called the operculum, forms inside the cervical canal during pregnancy. This provides a protective seal for the uterus against the entry of pathogens and leakage of uterine fluids. The mucus plug is also known to have antibacterial properties. This plug is released as the cervix dilates, either during the first stage of childbirth or shortly before. It is visible as a blood-tinged mucous discharge.
Childbirth
The cervix plays a major role in childbirth. As the fetus descends within the uterus in preparation for birth, the presenting part, usually the head, rests on and is supported by the cervix. As labour progresses, the cervix becomes softer and shorter, begins to dilate, and withdraws to face the anterior of the body. The support the cervix provides to the fetal head starts to give way when the uterus begins its contractions. During childbirth, the cervix must dilate to a diameter of more than 10 to accommodate the head of the fetus as it descends from the uterus to the vagina. In becoming wider, the cervix also becomes shorter, a phenomenon known as effacement.
Along with other factors, midwives and doctors use the extent of cervical dilation to assist decision-making during childbirth. Generally, the active first stage of labour, when the uterine contractions become strong and regular, The second phase of labor begins when the cervix has dilated to 10 cm, which is regarded as its fullest dilation, and is when active pushing and contractions push the baby along the birth canal leading to the birth of the baby. The number of past vaginal deliveries is a strong factor in influencing how rapidly the cervix can dilate in labour. The time taken for the cervix to dilate and efface is one factor used in reporting systems such as the Bishop score, used to recommend whether interventions such as a forceps delivery, induction, or Caesarean section should be used in childbirth.
Cervical incompetence is a condition in which shortening of the cervix due to dilation and thinning occurs before term pregnancy. Short cervical length is the strongest predictor of preterm birth.
Contraception
Several methods of contraception involve the cervix. Cervical diaphragms are reusable, firm-rimmed plastic devices inserted by a woman before intercourse that cover the cervix. Pressure against the walls of the vagina maintain the position of the diaphragm, and it acts as a physical barrier to prevent the entry of sperm into the uterus, preventing fertilisation. Cervical caps are a similar method, although they are smaller and adhere to the cervix by suction. Diaphragms and caps are often used in conjunction with spermicides. In one year, 12% of women using the diaphragm will undergo an unintended pregnancy, and with optimal use this falls to 6%. Efficacy rates are lower for the cap, with 18% of women undergoing an unintended pregnancy, and 10–13% with optimal use. Most types of progestogen-only pills are effective as a contraceptive because they thicken cervical mucus, making it difficult for sperm to pass along the cervical canal. In addition, they may also sometimes prevent ovulation.
Clinical significance
Cancer
Main article: Cervical cancer
In 2008, cervical cancer was the third-most common cancer in women worldwide, with rates varying geographically from less than one to more than 50 cases per 100,000 women. It is a leading cause of cancer-related death in poor countries, where delayed diagnosis leading to poor outcomes is common. The introduction of routine screening has resulted in fewer cases of (and deaths from) cervical cancer, however this has mainly taken place in developed countries. Most developing countries have limited or no screening, and 85% of the global burden occurs there.
Cervical cancer nearly always involves human papillomavirus (HPV) infection. HPV vaccines, such as Gardasil and Cervarix, reduce the incidence of cervical cancer, by inoculating against the viral strains involved in cancer development.
Potentially precancerous changes in the cervix can be detected by cervical screening, using methods including a Pap smear (also called a cervical smear), in which epithelial cells are scraped from the surface of the cervix and examined under a microscope. In some parts of the developed world, including the UK, the Pap test has been superseded with liquid-based cytology.
An inexpensive, cost-effective and practical alternative in poorer countries is visual inspection with acetic acid (VIA). Instituting and sustaining cytology-based programs in these regions can be difficult, due to the need for trained personnel, equipment and facilities and difficulties in follow-up. With VIA, results and treatment can be available on the same day. As a screening test, VIA is comparable to cervical cytology in accurately identifying precancerous lesions.
A result of dysplasia is usually further investigated, such as by taking a cone biopsy, which may also remove the cancerous lesion. Most cases of cervical cancer are detected in this way, without having caused any symptoms. When symptoms occur, they may include vaginal bleeding, discharge, or discomfort.
Inflammation
Main article: Cervicitis
Inflammation of the cervix is referred to as cervicitis. This inflammation may be of the endocervix or ectocervix. When associated with the endocervix, it is associated with a mucous vaginal discharge and sexually transmitted infections such as chlamydia and gonorrhoea. Other causes include overgrowth of the commensal flora of the vagina. When associated with the ectocervix, inflammation may be caused by the herpes simplex virus. Inflammation is often investigated through directly visualising the cervix using a speculum, which may appear whiteish due to exudate, and by taking a Pap smear and examining for causal bacteria. Special tests may be used to identify particular bacteria. If the inflammation is due to a bacterium, then antibiotics may be given as treatment.
Anatomical abnormalities
Cervical stenosis is an abnormally narrow cervical canal, typically associated with trauma caused by removal of tissue for investigation or treatment of cancer, or cervical cancer itself. Diethylstilbestrol, used from 1938 to 1971 to prevent preterm labour and miscarriage, is also strongly associated with the development of cervical stenosis and other abnormalities in the daughters of the exposed women. Other abnormalities include: vaginal adenosis, in which the squamous epithelium of the ectocervix becomes columnar; cancers such as clear cell adenocarcinomas; cervical ridges and hoods; and development of a cockscomb cervix appearance, which is the condition wherein, as the name suggests, the cervix of the uterus is shaped like a cockscomb. About one-third of women born to diethylstilbestrol-treated mothers (i.e., in-utero exposure) develop a cockscomb cervix.
Enlarged folds or ridges of cervical stroma (fibrous tissues) and epithelium constitute a cockscomb cervix. Similarly, cockscomb polyps lining the cervix are usually considered or grouped into the same overarching description. It is in and of itself considered a benign abnormality; its presence, however, is usually indicative of DES exposure, and as such, women who experience these abnormalities should be aware of their increased risk of associated pathologies.
Cervical agenesis is a rare congenital condition in which the cervix completely fails to develop, often associated with the concurrent failure of the vagina to develop. Other congenital cervical abnormalities exist, often associated with abnormalities of the vagina and uterus. The cervix may be duplicated in situations such as bicornuate uterus and uterine didelphys.
Cervical polyps, which are benign overgrowths of endocervical tissue, if present, may cause bleeding, or a benign overgrowth may be present in the cervical canal. Cervical ectropion refers to the horizontal overgrowth of the endocervical columnar lining in a one-cell-thick layer over the ectocervix.
Animals
Female marsupials have paired uteri and cervices. Most eutherian (placental) mammal species have a single cervix and a single, bipartite or bicornuate uterus. Lagomorphs, rodents, aardvarks, and hyraxes have a duplex uterus and two cervices. Lagomorphs and rodents share many morphological characteristics and are grouped together in the clade Glires. Anteaters of the family Myrmecophagidae are unusual in that they lack a defined cervix; they are thought to have lost the characteristic rather than other mammals developing a cervix on more than one lineage. In domestic pigs, the cervix contains a series of five interdigitating pads that hold the boar's corkscrew-shaped penis during copulation.
Etymology and pronunciation
The word cervix () came to English from Latin cervīx, which means "neck". Like its English translation, the Latin word can refer not only to the neck [of the body], but also to an analogous narrowed part of an object. Thus, the term cervix uteri (literally "neck of the uterus") is used in Latin to refer to the uterine cervix, but in English, the word cervix used alone usually refers to it. The first attested use of the word in English to refer to the cervix of the uterus was in 1702. The adjective cervical may refer either to the neck (as in cervical vertebrae or cervical lymph nodes) or to the uterine cervix (as in cervical cap or cervical cancer).
The Latin word cervix was in turn used to translate the Greek word αὐχήν (grc), "neck". The cervix was documented in anatomical literature in at least the time of Hippocrates; cervical cancer was first described more than 2,000 years ago, with descriptions provided by both Hippocrates and Aretaeus. Greek writers usually used the term στόμαχος (grc) to refer to the cervical canal; however, there was some variation in the sense of these two words.
References
Citations
Cited texts
References
- (2017). "Anatomy of the uterine cervix and the transformation zone". International Agency for Research on Cancer.
- (29 December 2011). "Human Papillomavirus (HPV) Vaccines".
- (2005). "Gray's Anatomy for Students". Elsevier/Churchill Livingstone.
- (2013). "Netter's Essential Histology". Elsevier/Saunders.
- (1995). "Gray's Anatomy". [[Churchill Livingstone]].
- (1969). "Anatomy: A Regional Study of Human Structure". W.B. Saunders.
- (2002). "Blaustein's Pathology of the Female Genital Tract". Springer.
- (2011). "Manual of Obstretics, 3/e". Elsevier.
- (2005). "The Cervix". Blackwell Publishing.
- (1994). "Blaustein's Pathology of the Female Genital Tract". Springer New York.
- (2011). "Anatomy of the uterus". Anaesthesia & Intensive Care Medicine.
- (2006). "Taking charge of your fertility: the definitive guide to natural birth control, pregnancy achievement, and reproductive health". Collins.
- (2009). "Larsen's human embryology". Churchill Livingstone/Elsevier.
- (November 2006). "The Cervix". Wiley-Blackwell.
- (October 2014). "The developmental origin of cervical and vaginal epithelium and their clinical consequences: a systematic review". Journal of Lower Genital Tract Disease.
- (2006). "Wheater's functional histology: a text and colour atlas". Churchill Livingstone/Elsevier.
- (December 2008). "Transformation zone (TZ) and cervical excision types". Cytopathology.
- (June 2005). "Audit of the histological definition of cervical transformation zone". Journal of Clinical Pathology.
- (2005). "Textbook of Medical Physiology". W.B. Saunders.
- (4 January 2014). "Demystifying IUI, ICI, IVI and IVF". Seattle Sperm Bank.
- (2008). "Sperm Transport and Capacitation". The Global Library of Women's Medicine.
- (November 2011). "The human female orgasm: a critical evaluation of its proposed reproductive functions". Sexual and Relationship Therapy.
- (March 2012). "The role of oxytocin in mating and pregnancy". Hormones and Behavior.
- (2014). "'Fertility Awareness-Based Methods' and subfertility: a systematic review". Facts, Views & Vision in ObGyn.
- (2021). "Anatomy, Histology, Cytology, and Colposcopy of the Cervix". Springer International Publishing.
- (2006). "The Cervix". Blackwell Publishing.
- (2022-09-12). "Functional evaluation of the cystic fibrosis transmembrane conductance regulator in the endocervix". Biology of Reproduction.
- Moghissi, Kamran S.. (1966-09-01). "Cyclic Changes of Cervical Mucus in Normal and Progestin-Treated Women". Fertility and Sterility.
- (November 2004). "Are vaginal symptoms ever normal? a review of the literature". MedGenMed.
- (May 2009). "The cervical mucus plug: structured review of the literature". Acta Obstetricia et Gynecologica Scandinavica.
- (2006). "Maternity Nursing". Elsevier Mosby.
- NICE (2007). Section 1.6, ''Normal labour: first stage''
- NICE (2007). Section 1.7, ''Normal labour: second stage''
- ACOG. (2012). "Obstetric Data Definitions Issues and Rationale for Change". Revitalize.
- (October 2004). "Planned caesarean section decreases the risk of adverse perinatal outcome due to both labour and delivery complications in the Term Breech Trial". BJOG.
- (2005). "Williams obstetrics". McGraw-Hill Professional.
- (January 2008). "Epidemiology and causes of preterm birth". Lancet.
- NSW Family Planning. (2009). "Contraception: healthy choices: a contraceptive clinic in a book". UNSW Press.
- (May 2011). "Contraceptive failure in the United States". Contraception.
- (May–Jun 1993). "Contraceptive efficacy of the diaphragm, the sponge and the cervical cap". Family Planning Perspectives.
- "Your Guide to the progesterone-one pill". Family Planning Association (UK).
- (January 2014). "Your Guide to the combined pill". Family Planning Association (UK).
- (December 2011). "Worldwide burden of cervical cancer in 2008". Annals of Oncology.
- World Health Organization. (February 2014). "Fact sheet No. 297: Cancer".
- (October 2013). "Worldwide trends in cervical cancer incidence: impact of screening against changes in disease risk factors". European Journal of Cancer.
- (2007). "Hardcore pathology". Lippincott Williams & Wilkins.
- (2005). "Human histology". Elsevier Mosby.
- (2008). "Harrison's Principles of Internal Medicine". McGraw-Hill Medical.
- (November 2010). "Different strokes: Pap-test and Babes method are not one and the same". Diagnostic Cytopathology.
- (2010). "Diagnostic Cytopathology". Churchill Livingstone.
- (September 2009). "Evidence-based, alternative cervical cancer screening approaches in low-resource settings". International Perspectives on Sexual and Reproductive Health.
- (2010). "Davidson's Principles and Practice of Medicine". Churchill Livingstone/Elsevier.
- (2013). "The Practitioner's Handbook for the Management of Sexually Transmitted Diseases". Seattle STD/HIV Prevention Training Center.
- (2014). "Comprehensive neonatal nursing care". Springer Publishing Company, LLC.
- (2007). "Robbins basic pathology". Saunders/Elsevier.
- (2008). "Harrison's Principles of Internal Medicine". McGraw-Hill Medical.
- (2002). "Cervical Stenosis: A Challenging Clinical Entity". Journal of Gynecologic Surgery.
- (February 2011). "Abnormal cervical appearance: what to do, when to worry?". Mayo Clinic Proceedings.
- "Diethylstilbestrol (DES) Cervix". National Cancer Institute.
- (June 1991). "The daughters of stilboestrol". BMJ.
- (June 1995). "Teratogen update: carcinogenesis and teratogenesis associated with exposure to diethylstilbestrol (DES) in utero". Teratology.
- (February 1975). "Prenatal exposure to stilbestrol. A prospective comparison of exposed female offspring with unexposed controls". The New England Journal of Medicine.
- (December 1997). "Congenital cervical atresia: report of seven cases and review of the literature". American Journal of Obstetrics and Gynecology.
- (June 2004). "The diagnosis and reproductive outcome after surgical treatment of the complete septate uterus, duplicated cervix and vaginal septum". American Journal of Obstetrics and Gynecology.
- (2005). "Life of Marsupials". Csiro Publishing.
- (30 January 1987). "Reproductive Physiology of Marsupials". Cambridge University Press.
- (2007). "Mammalogy: Adaptation, Diversity, Ecology". JHU Press.
- (September 1986). "Higher-Level Relationships of the Recent Eutherian Orders: Morphological Evidence". Cladistics.
- "The Female - Swine Reproduction".
- "Cervix". Etymology Online.
- (2011). "Galen: On Diseases and Symptoms". Cambridge University Press.
- (May 2009). "Cervical cancer: from Hippocrates through Rigoni-Stern to zur Hausen". Vaccine.
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Cervix — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report